“The way cancer looks hasn’t changed over the past decade, but what has changed is the detail and complexity of the information we can get from a biopsy. The biopsy—also known as taking a tissue sample—is one of the most important tools for an oncology to gain the insight needed to plan treatment. These days, biopsy methods are quite refined. The fine needle biopsy, for example, greatly reduces the pain, scarring, and complications for the patient than going with a scalpel to extract a tissue sample. But we have our work cut out for us in correctly identifying the type of cancer from such a small sample. Keeping such a tiny tissue sample viable, for further testing, is not easy either.” [Assistant Professor Samornmas Kanngurn] said, giving a snapshot of the work of the surgical pathology department at Bumrungrad Hospital.
Signposting the treatment paths
“The main job of a surgical pathologist is to diagnose the patient’s illness from the tissue samples provided by the patient using a microscope.
 According to the medical code of conduct, every kind of tissue removed from human body must be sent to us for a pathological examination, even ones that looks harmless. If a patient is suffering from abdominal pain, and appendicitis is suspected
According to the medical code of conduct, every kind of tissue removed from human body must be sent to us for a pathological examination, even ones that looks harmless. If a patient is suffering from abdominal pain, and appendicitis is suspected, we will examine the removed appendix to confirm the diagnosis and see whether any other diseases or conditions are present. In rare cases, an appendicitis can coexist with cancer of the appendix. Another example is with polyps found in the large intestine of the patient. These abnormal tissue growths are usually benign, but through biopsies we had caught bowel cancer in the early stages from such samples. And of course, for any cancer to be confirmed, a biopsy must be performed and microscopically diagnosed by pathologist.”
“When an abnormal tissue growth is discovered, the doctor will usually send the patient for a biopsy before an informed decision on the next steps for treatment can be made. For example, a sample of tissue from the breast lump will be extracted using a fine needle. The sample, about 1-2 centimeters long and no more than 2 millimeters wide, is then sent to the pathologists to determine whether it is benign or malignant. Patients with benign tumors may require only a simple surgery to remove the tumor. But a malignant tumor—
breast cancer, in other words—is more complicated to operate on, and will require a partial or
complete mastectomy and lymph node biopsy to completely stage cancer."
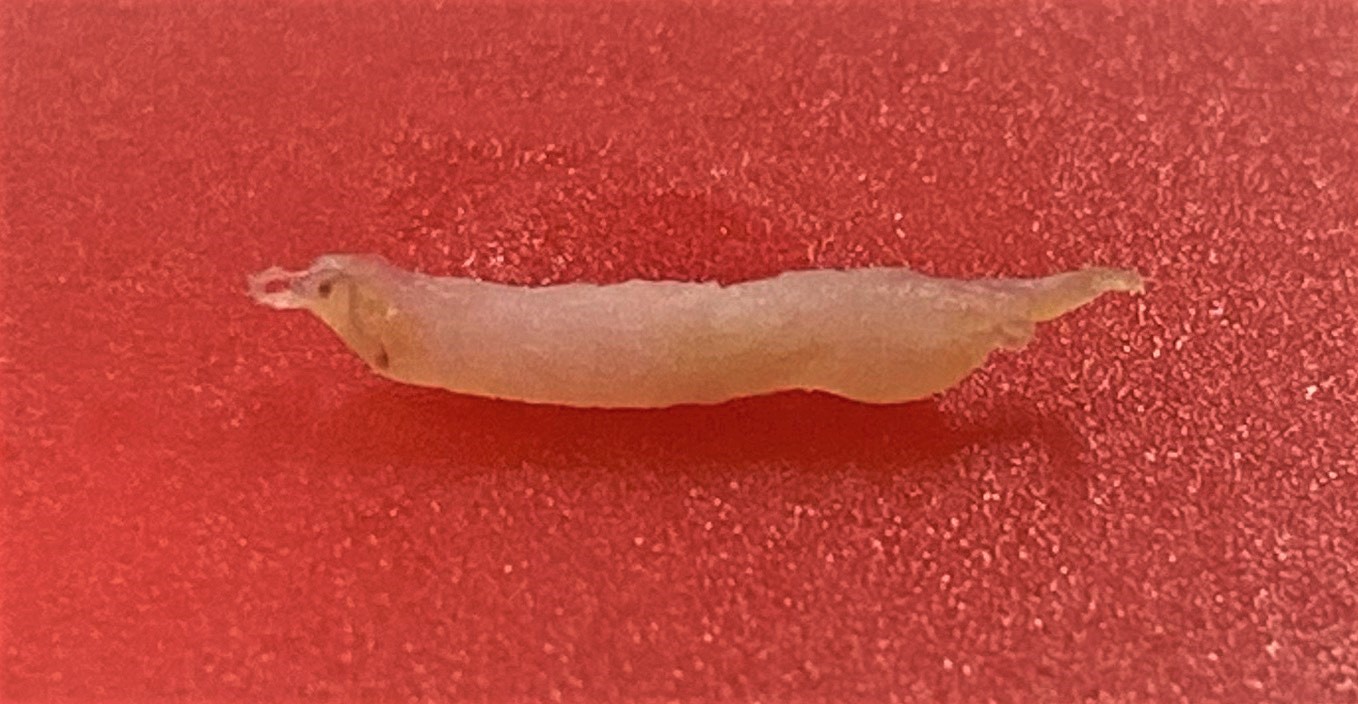
Smaller samples call for greater care
Dr. Samornmas further explains the principles of biopsy for diagnosis and treatment: “The tissue samples, whether they’re meters or millimeters long, will be processed until they can fit on to the small glass slides, just 3 microns thick.
The surgical pathologists will examine these under a microscope to identify the pathology of the tissue. The remaining tissue will be embedded in a paraffin block and stored for at least ten years as mandatory.

If further tests are needed, such as immunohistochemistry or
genetic profiling, we can just take another slice from that paraffin embedded tissue. The problem that we face is that the tissue samples are so small, and the particularly cancer patients today often require many different kinds of tests, such as molecular tests for
targeted therapy or i
mmunotherapy. And it just wouldn’t do to subject the patient to biopsy after biopsy, because we didn’t get enough tissue in the first place.
This gives the pathologist an extra responsibility; that of determining in advance how much tissue to take as a sample. These appraisals are made together with the
oncologists, so as to minimize the number of times the patient will have to undergo a biopsy. In cases where we are unsure, we have ways of performing rapid tests during biopsy to confirm how much tissue is actually needed.”
Ongoing improvement
“
Our pathology laboratory is the first private hospital laboratory in Thailand to be certified by the College of American Pathologists (CAP). This gives our medical teams and our patients a great deal of confidence in our lab processes and, ultimately, the test results that come out of our lab. We always work as a team. If there is a slide that is particularly hard to make a diagnosis with, we will seek the professional opinion of other pathologists or relevant specialists.
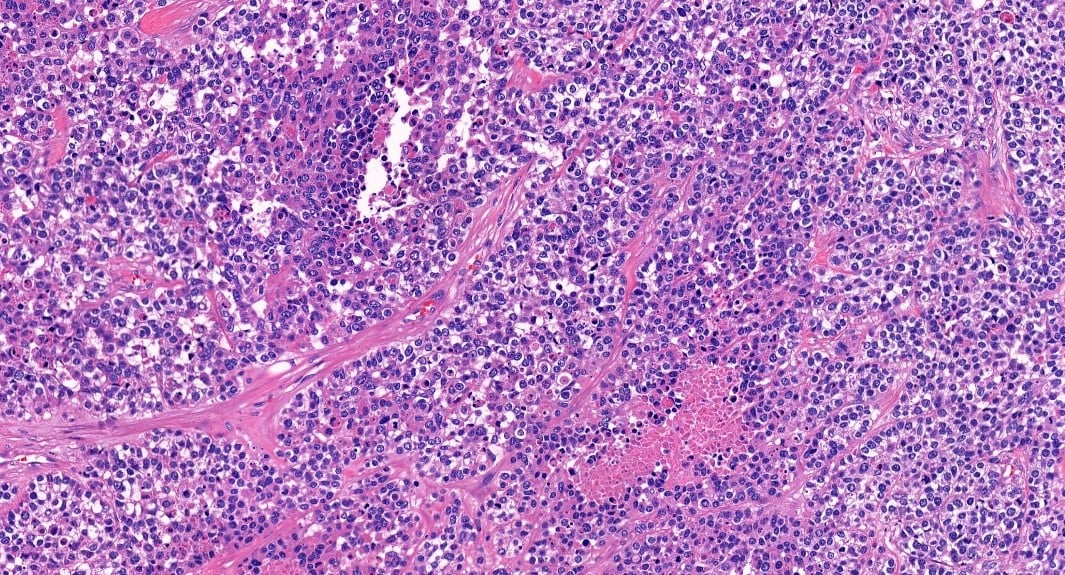
We also employ digital pathology technology, which can process data in a way that helps us to gain an extremely accurate insight of cancer at microscopic level. For example, the cell-counting module is instrumental in helping us to quickly identify
patients who will benefit from hormone therapy”
To answer a curious mind
“Pathologists rarely see patients face to face, because we usually do our diagnostics work with the tissue samples. But patients sometimes have questions about the test results that only a pathologist can answer. Ever since I started working at Bumrungrad Hospital, I’ve fielded all kinds of questions from patients. Using my expertise to give them answers goes some way to putting their minds at rest. I sometimes still receive updates about patients and former patients from their relatives.”
Been there and done that
“I myself was once a cancer patient at Horizon Regional Cancer Center. Six years have passed, and I still get regular checkups. I follow my doctor’s recommendations and take my anti-hormone medicine rigorously
. I keep by body fit and strong and if I didn’t tell anybody, no one would be able to tell that I’ve been through cancer. I want to tell other cancer patients that there is always hope. Cancer is not a death sentence. I’m still here, happily living my life after all that. I’ve seen with my own eyes how many cancer patients pull through this, and go on to live happy and fulfilling lives, because they never lost hope and kept on fighting,” Dr. Samornmas said in closing with this very personal study in positivity and perseverance.
For more information please contact:
Last modify: August 30, 2023