“When we’re caring for cancer patients, one of the hardest things to do is to find the blood vessels for chemotherapy. This is because they’ve already had so many injections and intravenous drips that the remaining viable blood vessels are few and far between. This is why we urge the doctors to opt for a central line to administer medication, so that their pain and suffering is minimized.” This is a small example of the enduring thoughtfulness from Kannika Boonprachom, the Oncology Nurse Manager at the Horizon Regional Cancer Center.
Being an oncology nurse entails communicating with cancer patients throughout the entirety of their treatment. Whether it be details concerning their treatment plan, information regarding the disease they are facing, expenses, or post-treatment follow-ups, the oncology nurses are more often than not the ones to relay crucial information between the patients and doctors.
“As per the fundamental tenets of a hospital, we do everything to ensure the safety and comfort of our patients. But above and beyond that, we really put our hearts into making the treatment experience as warm and humane as possible, which benefits the nurses as much as it does the patients,” Kannika explains. “The closer we are to our patients, the better the moral support that we can give. Ultimately, this leads to better treatment results.”
Being observant is a survival skill that we practice for our patients
“Patients who have been through treatment but are still waiting to be declared free of cancer are often the most anxious. They tend worry that they aren’t completely cured, or that they could be doing something wrong that would allow the cancer to return. We have to be extra observant and be ready to give good advice. For example, if a patient is experiencing nausea, we have to refer back to the day that they received their medication and what that medication was. This is so that we can react quickly and inform the doctors, or arrange for the pharmacists come and explain to the patient,” Kannika details. “If we notice that a patient is not finishing their meals, we go to the nutritionist immediately with the details of which foods they’ve been eating or leaving. The nutritionist can then figure out a way to ensure that the patient is at least receiving food that can eat to keep them strong and in good spirits throughout their treatment!”
The nature of cancer treatment means that oncology nurses must constantly liaise with a diverse range of disciplines and people. “In the case conferences we bring our most challenging cases into the discussion. In this way, we learn from each other, such as different ways of keeping patients’ spirits up, or how best to deal with the various other situations that arise. We share our techniques and best practices with each other so that all the oncology nurses are of equal readiness for our patients.”
Kannika also went into the finer details of the oncology nurse’s job, such the administration of
chemotherapy, and the various types of blood cells and plasma infusions for patients with a low blood count. “The ability to find viable blood vessels is a skill that cannot be overstated. The patients are constantly receiving injections of some kind or another, so their blood vessels shrink and retract as a result. It takes real skill to find the remaining blood vessels, which sometimes requires aids such as tourniquets or warm compresses. For particularly difficult cases, the hospital’s dedicated IV Team must be called in.”
We want to help ease the pain
“Every time we see our patients suffering from the pain, for example when we’re trying to find a good blood vessel, it pains us too. It wouldn’t be so bad if it was only once in a while, but it is a constant occurrence for cancer patients,” Kannika confesses.
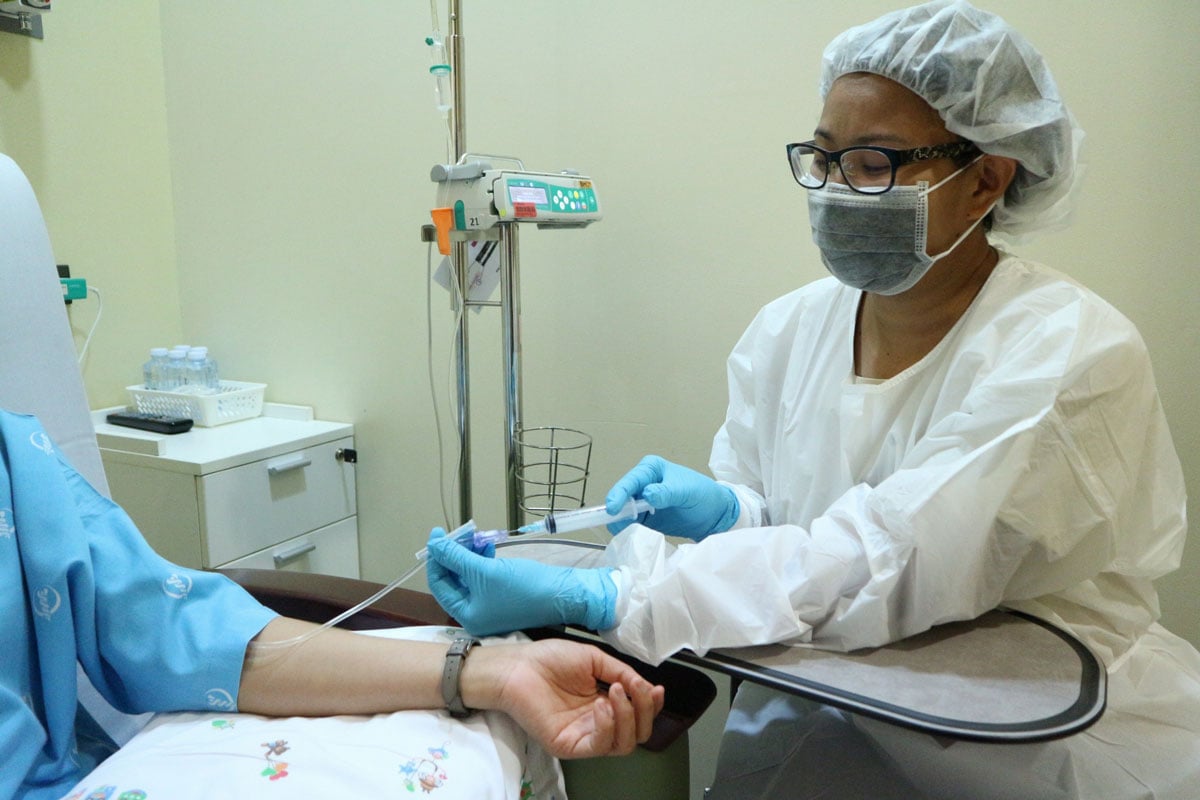
“Not onlythat, but the medications themselves so potent that if the blood vessel ruptured, the medication could actually kill some of the surrounding muscle tissue. This is why we make a thorough assessment and seek the doctor’s permission for a central line whenever possible.”
Inserting a central line, also known as a central venous catheter (CVC), is a way to avoid piercing a blood vessel each time medication must be given. The targeting of the central line is also more direct. “When a central line is installed, all the nurse has to do to administer medication or draw blood is to insert a needle into the tubing rather than into the patient. The patient feels no pain from the needle at all. We are good enough at this that we have never had a single clogged tube,” Kannika beamed with no small amount of pride.
Hope for the future
“As nurses, everything that we do for our patients comes from the heart. We want to tell every single cancer patient that new advances are being made every day; we want all our patients to stay strong and positive. We do our best to be as comforting and attentive as possible. Every time one of our patients is able to smile, the positive energy of that smile feedbacks from us to all of our other patients too. Every hug, the warmth from every hand that is held, it all gets passed around,” said Kannika on behalf of all the oncology nurses at the
Horizon Regional Cancer Center.
For more information please contact:
Last modify: September 01, 2023