Incidence and Importance
An ankle sprain is considered one of the most common injuries among musculoskeletal injuries, requiring a trip to the emergency room for medical help. Mostly found in the 15-35 years old group, the incidence of lateral ankle sprain stands at 0.54-11.55 per 1,000 exposures.
A sprained ankle is of importance as an acute injury resulting in complete ligament rupture has been found to cause disabilities in approximately 20% of general patients and possibly as many as 40% of athlete patients. The disabilities include ankle instability and recurrent sprains, which can lead to damaged ankle cartilage, altered biomechanics, and a high risk of arthritis of the ankle joint in the long-term follow-up.
Physical examinations
Anterior drawer test (Fig. 1)
This is done to determine if the ATFL can still limit anterior displacement of the talus properly. The test result is considered positive if there is greater than 5 mm of anterior motion over the other ankle, or more than 10 mm when examining only one ankle. A suction sign over the area of ATFL also indicates a positive test result.

Fig. 1 depicts a lax ankle, with the anterior drawer test showing a positive suction sign.
Talar tilt test (Fig. 2) This is done to determine if the CFL can still prevent an excessive inversion of the talus.
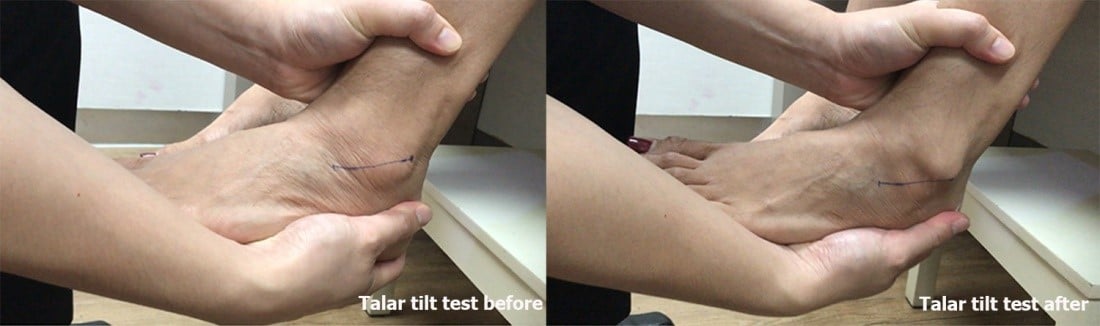
Fig. 2 depicts a lax ankle,
with a positive talar tilt test showing clearly identify at the tip of the distal fibula.
Investigation (Further tests for diagnosis)
Magnetic resonance imaging (MRI)
The
MRI has been found to be more accurate in diagnosing acute ligament rupture than chronic ligament rupture, with 74% accuracy for partial tear and 79% for complete tear.
Ligament injury classification
Lateral ankle ligament rupture can be divided into three grades according to the levels of severity as follows:
- Grade 1: Mild sprain with no ligament rupture
- Grade 2: Moderate sprain with partial rupture of ligament
- Grade 3: Severe sprain with complete rupture of ligament
Treatment
Functional management: This mainly entails early mobilization, getting the patient to move the ankle right after the injury in weight-bearing walking with external support and continue with physical therapy until the patient recovers.
Operative treatment
The objective of the surgery is for lateral ankle ligament reconstruction to increase ankle stability, reduce pain or swelling, allowing the patient to return to normal daily activities or sports practices.
Indications for surgery include ankle instability and/or a swollen ankle even after complete conservative treatment for at least 3-6 months.
Regarding surgical techniques for lateral ankle ligament reconstruction, both open repair and arthroscopic repair are possible.
The standard open repair allows the surgeon to have a full view of the ligaments and the tip of the distal fibula. Effectively repaired in this way, the ligaments can be very strong with the largest number of suture threads used in the ligament repair and the sutures being made efficiently. Adding artificial ligaments can also be considered to strengthen the ankle ligaments on the outside as the artificial ones are four times stronger than the natural ligaments.
However, with large surgical wound, the open repair has some disadvantages. Compared to the arthroscopic repair, the risk of infection is higher, the scar is bigger and more prominent with less pleasing appearance, post-surgical pain level is higher, and the recovery time is longer.
The arthroscopic repair has now become more popular, compared to the open repair, due to the smaller surgical wounds, which helps reduce post-surgical pain and infection risk. Also, the scar is of more pleasing appearance and recovery time is shorter.
On the other hand, a major complication with the arthroscopic repair is cutaneous nerve injury in 3-10% of the cases. This is because with the arthroscopy, the nerves remain unseen. The injured nerves can cause numbness or pain in the sides of the feet and ankles. And while the ankle is strengthened enough for the patient to do daily activities or play sports, it is not as strong as the outcome achieved in an open surgery.
Compiled by Lt.Col.
Dr. Chamnanni Rungprai, Orthopaedic surgeon,Foot & Ankle Surgery
For more information please contact:
Last modify: April 22, 2025