How does cervical spine degeneration occur and why does it result in nerve compression?
Cervical spine degeneration can occur due to aging and usage as this part of the spine is responsible for carrying the weight of the head and requires constant movement. Degeneration can affect anyone, although the degree of degeneration varies from person to person
The degeneration of the cervical spine begins with the degeneration of the intervertebral discs. This is followed by the degeneration of the facet joints and uncovertebral joints. As the degeneration progresses, the joints may become swollen or unstable, leading to chronic neck pain that comes and goes, while some individuals may not experience neck pain but experience stiffness in the region. Over time, the body responds to these changes by attempting to build new bone in the joints or other parts of the spine that are involved in movement. The newly formed bone is referred to as bone spurs or osteophytes, which reduce the range of motion but often ease neck pain, with some individuals not having any neck pain at all at this point. However, these bone spurs or osteophytes can compress or irritate nearby nerves, causing symptoms such as radiating arm pain along the pathway of the affected nerve. In younger patients, nerve compression due to bone spurs is less common because the cervical spine is less degenerated, though it can still occur due to the degeneration of the intervertebral discs, which is most commonly seen in individuals between the ages of 30 to 50.
Factors that can accelerate cervical spine degeneration
- Smoking: This can cause stenosis in blood vessels that service the spinal region.
- Usage: Improper postures and behaviors, such as hunching over while writing or staring at a computer screen for extended periods, sleeping with excessively high pillows, or engaging in activities like reading or watching TV while lying down, or tilting the head forward to work, such as automobile mechanics working under a car, can all cause the neck to be in an abnormal position for an extended period. Consistent exposure to these improper postures and behaviors can accelerate cervical spine degeneration.
- Being in an accident: Being involved in a car or motorcycle accident can result in the cervical spine being impacted or experiencing severe twisting, which can cause tearing or dislocation of the intervertebral discs or joints.
- Certain sports: Dangerous activities include, for example, heading the ball while playing soccer or playing American football, both of which involve frequent impacts to the head or neck, in addition to practicing certain yoga poses, such as headstands, where the weight of the body is supported by the neck.
Symptoms associated with cervical spine degeneration
- No noticeable symptoms may be present, although there may be occasional neck discomfort that comes and goes without being treated.
- Chronic neck pain may improve with pain medication, but then return. Some individuals may experience shoulder pain or discomfort radiating down to the scapular or shoulders when tilting the neck.
- Neck pain that radiates down to the arms indicates that cervical spine degeneration is starting to compress the nerves. There may be a history of sudden shooting pain from the neck to the elbow or fingers, causing a momentary jolt. Subsequently, there may be a reduction in shooting pain, but tingling and arm weakness may be felt, with the arm becoming weak.
- No neck pain may be present, but there may be shoulder discomfort, which may or may not be accompanied by numbness.
- Walking unsteadily or feeling weakness in the limbs without neck pain (cervical myelopathy) may be experienced. If the nerve compression is severe, it can cause difficulty in walking or controlling bowel and bladder functions.
Diagnosis
- X-ray cervical spine
- MRI cervical spine
Treating cervical spine degeneration
1. Conservative forms of treatment:
- Lying down flat to rest in order to relieve the cervical spine from bearing weight.
- Applying a hot pack to the neck area for 10-15 minutes.
- Using a soft collar or hard collar to support the neck where pain is severe, especially when the pain is acute in the first week.
- Taking pain relief medication, such as paracetamol, non-steroidal anti-inflammatory drugs (NSAIDs) or muscle relaxants. Topical pain-relieving creams or ointments may also be used. Any drugs should be taken with caution as they may irritate the stomach.
- Avoid massaging the neck during the acute pain phase as it may exacerbate the symptoms.
- Performing certain exercises and physical therapy to alleviate chronic neck pain should focus on increasing joint mobility in the cervical spine and strengthening the muscles around the neck. Keep the neck in a neutral position, place the hand above the ear on the opposite side, and gently pull the head to one side, resisting the movement by tensing the neck muscles without actually moving the neck or causing pain. Count from 1 to 10 and repeat 5 to 10 times per session, approximately 3 times a day. Another exercise involves placing the hand on the forehead to tense the forehead muscles and resisting by pushing against the hand, following the same method of counting and repetition. Practice these exercises frequently to strengthen the muscles in order to provide greater support to the cervical spine.
- Physical therapy in a hospital setting may include the use of heat therapy (ultrasound) or cervical traction treatment, which can help improve symptoms.
Preventing cervical spine degeneration
- Avoid exposure to risk factors, such as smoking.
- Be mindful of posture while working, avoiding excessive bending or tilting of the neck.
- Take regular breaks during work to exercise the neck muscles, move the neck, or change positions.
- Use a chair with adequate support to cushion the neck.
- When sleeping, use a pillow that supports the cervical spine, keeping the head from tilting or bending excessively.
- Engage in exercises to strengthen the neck muscles.
2. Surgical forms of treatment
Indicators:
-
Utilizing conservative forms of treatment for up to 6 weeks without seeing any improvements.
-
Experiencing persistent pain that impacts the ability to perform daily tasks.
-
Numbness or persistent weakness in the arms despite receiving treatment.
Is surgery dangerous?
It has been found that surgery for cervical spine degeneration with nerve compression is highly safe and effective. The surgical procedure has a success rate of 90-95%, with patients typically staying in hospital for no more than 2-3 days, often being able to stand, walk, and resume normal daily activities just a relatively short time after surgery.
What are the steps involved with surgery?
-
A surgical incision of approximately 3–5 cm in length is made on the front side of the neck.
-
The incision is made to access the interverbal discs and remove any bone spurs or herniated bone that is compressing the nerves.
-
The affected vertebrae are fused together by inserting a bone graft taken from the pelvic area or using artificial bone substitutes, which help alleviate pain caused by the removed bones. This fusion process ensures the stability and height of the fused vertebrae.
-
In some cases, metal hardware(plate) may be used to assist the fusion, especially when multiple vertebrae are involved. Titanium alloy is commonly used as it is non-corrosive and has minimal side effects, allowing it to be left in place indefinitely (see Figure C).
-
The fusion procedure may result in limitations in neck flexion, extension, or rotation. To address this, artificial spinal discs (disc prostheses) can be used as a substitute for fusion (see Figure D) as they allow for a return to a normal range of motion.
Recovery times
Typically, cervical spine surgery for degenerative conditions requires a hospital stay of around 2-3 days, with most patients able to return home after the procedure. Generally, pain improves immediately after the surgery, and patients are able to stand, walk, and resume daily activities straight away. However, some patients may need to use a neck collar initially to prevent excessive bending or extension of the neck following the surgery.
Article by Dr. Pritsanai Pruttikul
Specialist in Orthopedics and Spinal Surgery
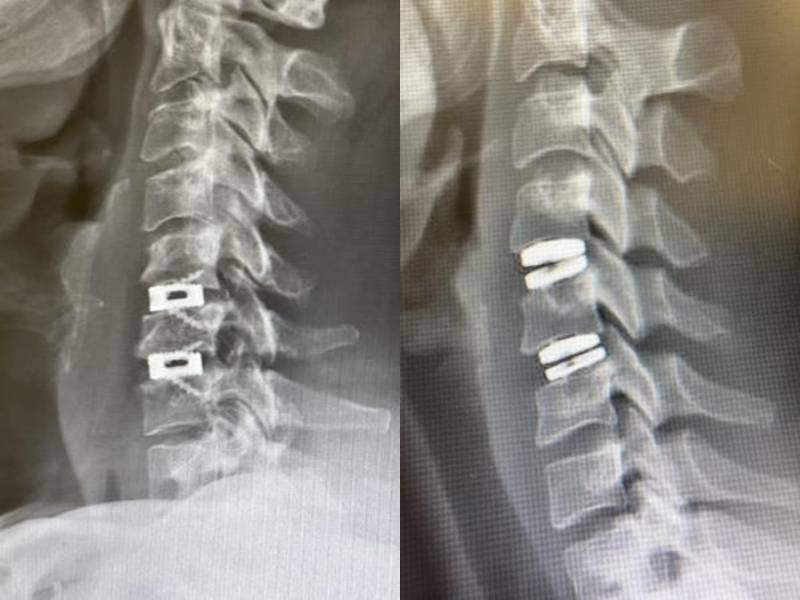
Images showing x-rays following spinal surgery, consisting of a spinal fusion procedure (left) and a flexible artificial spinal disc prosthesis procedure (right).
For more information please contact:
Last modify: November 30, 2024