Pharmacogenomics studies how your genes affect your response to drugs. In some cases, your genes can determine whether you might have adverse effects to a drug, or could tell whether this drug is effective for you. It is a very rapidly expanding part of precision medicine, which aims to customize health care, with decisions and treatments tailored to each individual in every way possible.
How does pharmacogenomics work?
Drugs interact with your body on different levels, depending on both how you take the drugs, and where they work in your body. After you take the drug, your body must break it down and deliver it to the targeted area. Your genes can affect numerous steps in this process to influence your response to the drug. Examples of interactions include:
- NUMBER AND TYPE OF DRUG RECEPTORS:
Our cells have a variety of receptors, which are macromolecules in the membrane or inside the cell. Some of them specifically bind a drug. Your genes determine what type of receptors you have and how many, which can affect your response to the drug. You might need a higher or lower dose of the drug than the majority of people, or your doctor might consider to prescribe you an alternative drug.
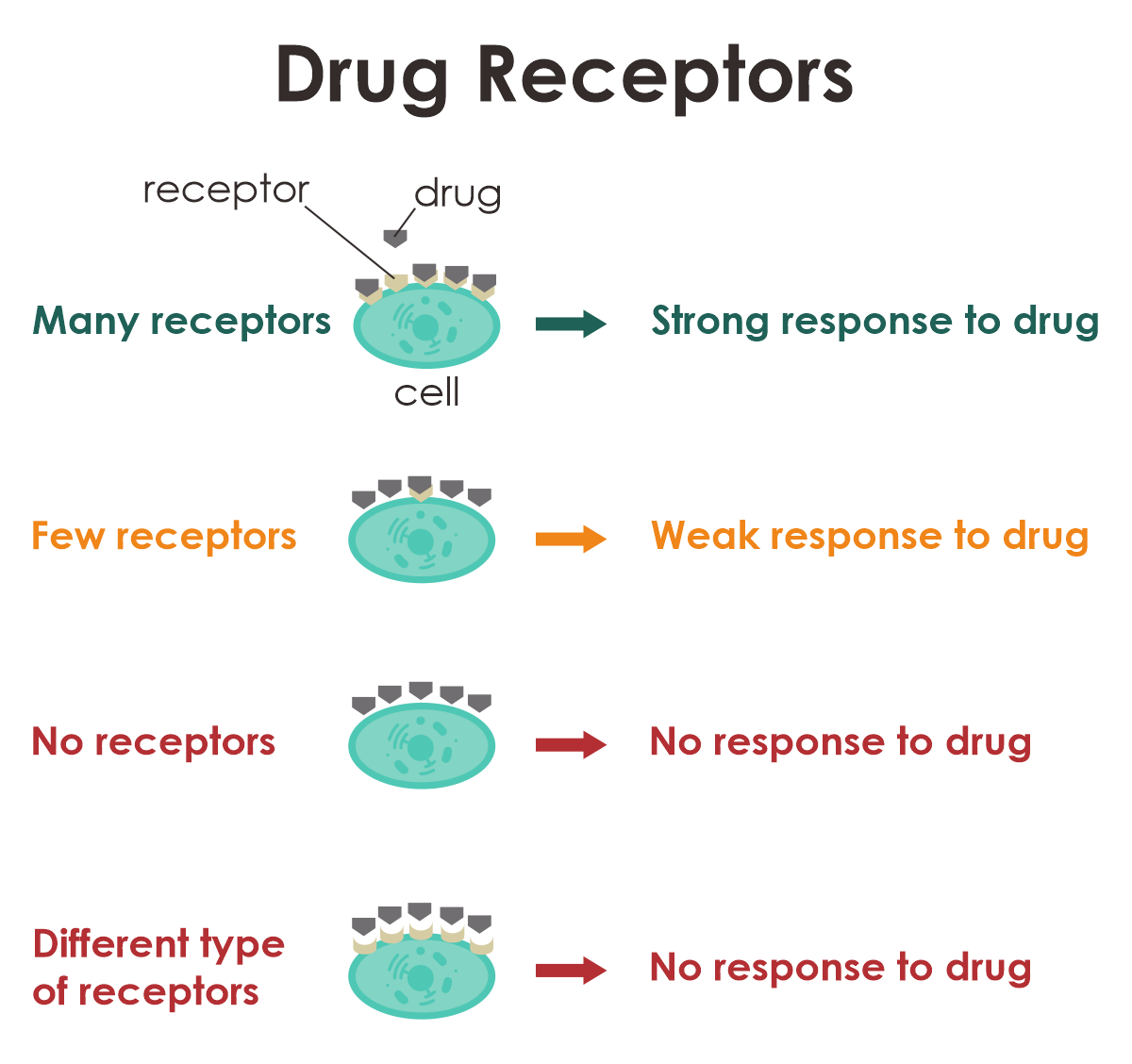
Example: Breast Cancer and Trastuzumab Emtansine (T-DM1)
Some breast cancer cells have many HER2 receptors, and this extra HER2 helps the cancer grow and spread. T-DM1 can be used to treat this type of breast cancer, because it can attach to HER2 receptors on cancerous cells, thereby killing them. If you have breast cancer, your doctor may test a sample of your breast tumor to check if T-DM1 is the right medication for you. If your cancer cells have a lot of HER2 receptors (HER2 positive), you doctor may prescribe T-DM1. But if your tumor does not have enough HER2 receptors (HER2 negative), T-DM1 will not work for you.
Some drugs need to be taken into the cells and tissues, where they specially act on. Your genes can affect uptake of particular drugs. Decreased uptake may lower the drug effectiveness and can cause accumulation in other parts of your body, which can lead to other problems. Your genes may also affect how quickly some drugs are removed from the cells in which they act. If drugs are removed from the cells too quickly, they might not have time to work.
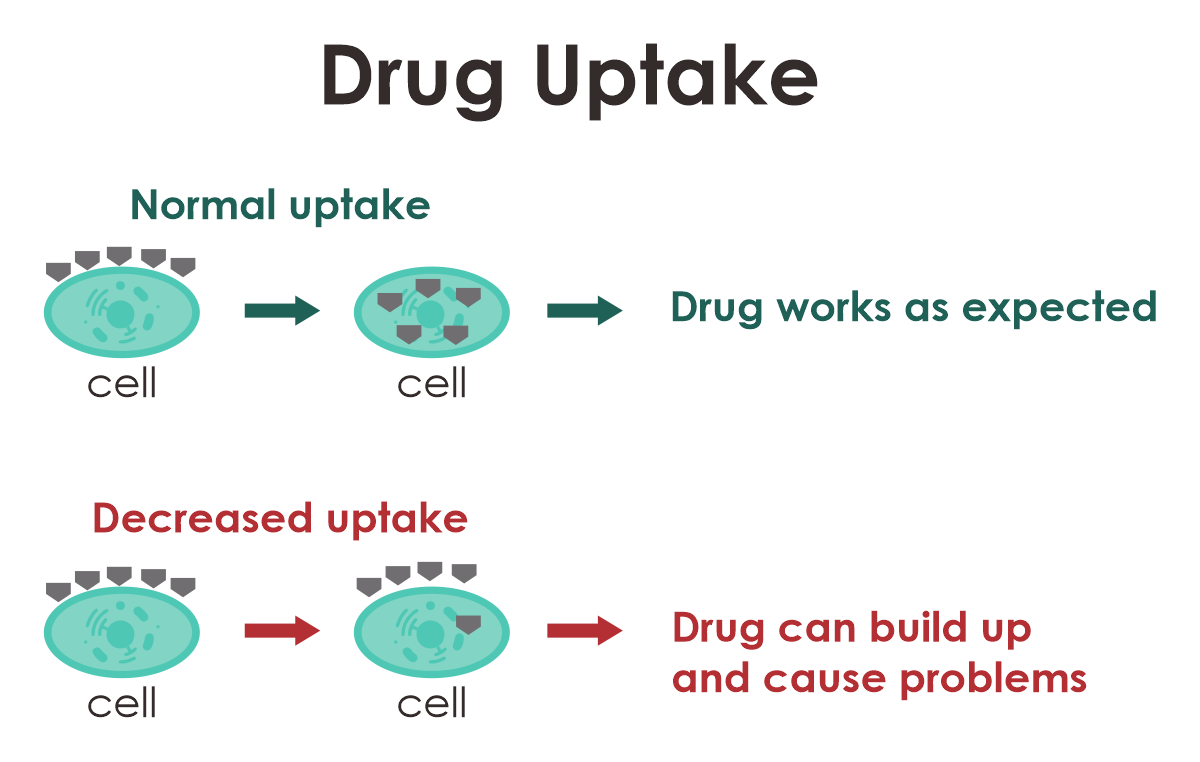
Example: Statins and Muscle Problems
Statins are drugs, which act in the liver to help lower the level of cholesterol. To work correctly, they must first be taken into the liver. Statins are transported into the liver by a protein made by the
SLCO1B1 gene. Some people have a specific change in this gene (single nucleotide variant or SNV), which affects the liver uptake of several statins. As a result, the concentration of such statins may build up in plasma, leading to so-called statin induced myopathy. This condition includes fatigue, muscle pain, muscle tenderness, muscle weakness, nocturnal cramping, and tendon pain. Before prescribing statins, your doctor may recommend a genetic testing for the
SLCO1B1 gene to adjust the statin dose for the best result or to identify the appropriate statin for you.
Your genes can affect the speed of breaking down drugs in your body. If you break down the drug quicker than the majority of people, your body could clear out the drug faster and you might need an increased dose of drug or even an alternative drug. If your body breaks down the drug more slowly, you might need a lower dose of drug.
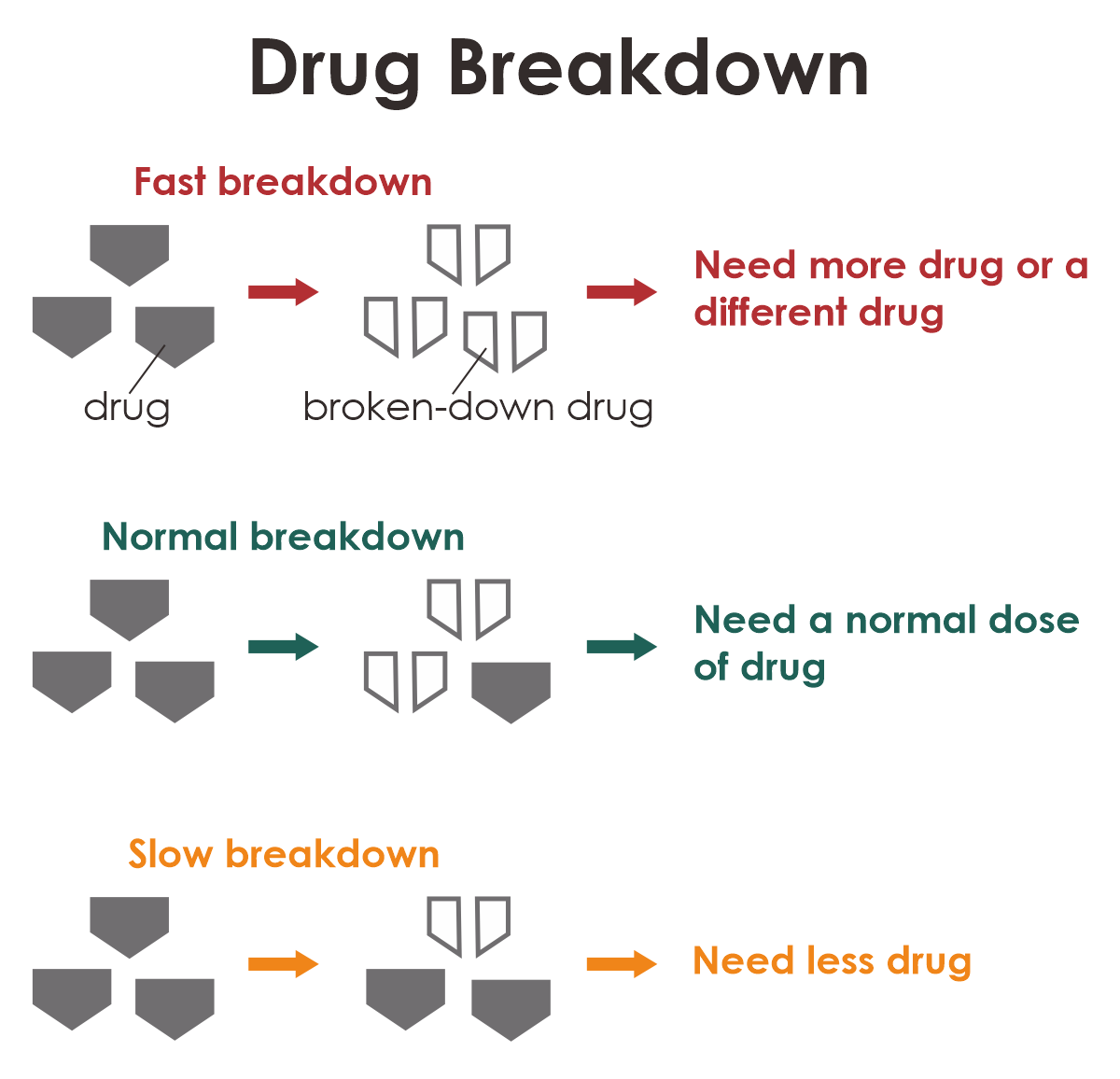
Example: Depression and Amitriptyline
The metabolism of the antidepressant drug amitriptyline is influenced by two genes called
CYP2D6 and
CYP2C19. Before prescribing amitriptyline, your doctor may recommend a genetic testing for the
CYP2D6 and
CYP2C19 genes, which helps to adjust the dose. If you break down amitriptyline too fast, you will need a higher dose, or you may need an alternative drug. If you break down amitriptyline very slowly, you will need to take a smaller dose or change it to an alternative drug to avoid adverse reactions.
- TARGETED DRUG DEVELOPMENT
Pharmacogenomics plays a crucial role in drug development. It helps to target the underlying problem rather than simply treating disease symptoms. Some diseases are caused by mutations in genes. The same gene can have different types of mutations, which have different effects. Some mutations may result in a defective protein, while others make no protein at all. Medications can be designed based on how the mutation affects the protein, and these drugs will only work for a specific type of mutation.
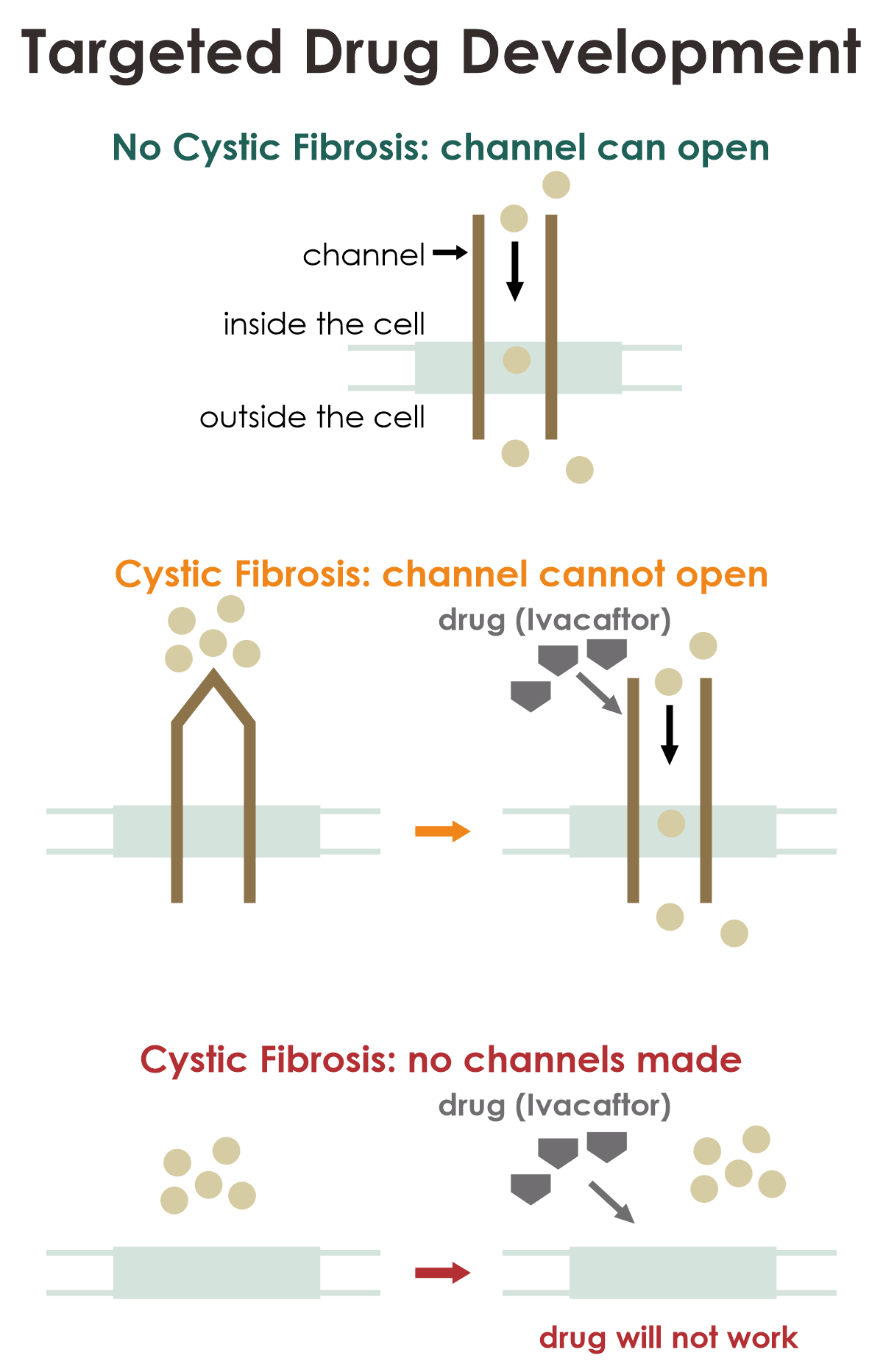
Example: Cystic Fibrosis and Ivacaftor
Cystic fibrosis is genetic disease caused by mutations in the cystic fibrosis transmembrane conductance regulator gene (
CFTR), which affect the CFTR protein. This protein forms a channel, which acts as a passageway to move particles called chloride ions into and out of cells. For most people such protein is made correctly, and the channel can open and close. However, some mutations in the
CFTR gene that cause cystic fibrosis result in a closed channel. Ivacaftor is the medication that can act on certain
CFTR mutations by opening the ion channel and improving the transport of chloride through the channel. Ivacaftor would not be expected to work for people with cystic fibrosis, whose mutations result in cells producing little or no CFTR protein.
What does this mean for your health?
Pharmacogenomic testing has become an essential tool for precision medicine and is currently used for prescribed drugs. Improved understanding of your pharmacogenomic profile can protect your health, explain past drug responses, guiding your current and future medication therapy. The Bumrungrad
Preventive Genomics and Family Check-up Services provide the pharmacogenomic testing and offer pharmacogenomic test result interpretation for patients, who may have already undergone testing elsewhere. Pharmacogenomic testing helps to adjust the dose, avoid adverse reactions, or select an alternative drug. The clinic is a collaborative, multidisciplinary practice that involves a medical geneticist, a clinical pharmacist, and a genetic nurse with specialized training in pharmacogenomics.
To schedule
an appointment with our world-class clinical team in the Preventive Genomics Services, call:
02-011-4890 or
02-011-4891
Individuals and referring providers interested in
an appointment can also contact our team by email at
[email protected]
For more information please contact:
Last modify: August 22, 2023